Periorbital cellulitis: Difference between revisions
(Created page with "===Background=== *Must distinguish between these orbital and periorbital cellulitis! **See Periorbital vs Orbital Cellulitis *Periorbital cellulitis most often 2/2 contiguous...") |
(Strip excess bold) |
||
| (30 intermediate revisions by 9 users not shown) | |||
| Line 1: | Line 1: | ||
==Background== | |||
[[File:Orbital septum slide - final big gallery.jpeg|thumb|Periorbital anatomy.]] | |||
*Also known as preseptal cellulitis — infection anterior to the orbital septum | |||
* | *Most often due to contiguous spread from [[sinusitis]], skin infection, insect bite, or local trauma | ||
* | *Most patients are <10 years old | ||
*Rarely progresses to [[orbital cellulitis]], but must be distinguished from it (see table below) | |||
*Common organisms: ''S. aureus'', ''S. pneumoniae'', ''S. pyogenes'', ''H. influenzae'' (in unvaccinated) | |||
{{Periorbital vs orbital cellulitis}} | |||
==Clinical Features== | |||
[[File:PMC3214412 IJO-59-431-g007.png|thumb|Periorbital cellulitis]]. | |||
*Eyelid swelling, erythema, tenderness, warmth | |||
*+/- [[fever]] | |||
*Key distinguishing features from [[orbital cellulitis]] (all ABSENT in preseptal): | |||
**[[Proptosis]] | |||
**[[red eye|Chemosis]] | |||
**Globe displacement | |||
**Limitation of extraocular movements | |||
**Pain with eye movement | |||
**[[Diplopia]] | |||
**[[Vision loss]] | |||
=== | ==Differential Diagnosis== | ||
{{Periorbital swelling DDX}} | |||
== | ==Evaluation== | ||
[[File:RtmaxobitinfectteethCT.png|thumb|Periorbital cellulitis caused by a dental infection (also causing maxillary [[sinusitis]]).]] | |||
*Visual acuity, pupil exam, extraocular movement assessment — essential to distinguish from orbital cellulitis | |||
*CT orbit with IV contrast if: | |||
**Equivocal exam (unable to fully assess proptosis, EOM, or pain with eye movement) | |||
**Unable to accurately assess vision (e.g. age <1 year) | |||
**Toxic-appearing or not improving on antibiotics | |||
**Concern for orbital abscess (subperiosteal or orbital) | |||
*Blood cultures if febrile or toxic-appearing | |||
==Management== | |||
{{Periorbital Cellulitis Antibiotics}} | |||
==Disposition== | ==Disposition== | ||
* | *Outpatient: Well-appearing, afebrile, mild disease, reliable follow-up in 24 hours | ||
** | *Admit: Age <1 year, toxic-appearing, febrile, unable to tolerate PO, failed outpatient therapy, concern for orbital involvement | ||
*Return precautions: Worsening swelling, fever, vision changes, pain with eye movement, inability to open eye | |||
==See Also== | ==See Also== | ||
*[[Periorbital | *[[Periorbital swelling]] | ||
*[[ | *[[Orbital cellulitis]] | ||
==References== | |||
<references/> | |||
[[Category:ID]] | [[Category:ID]] | ||
[[Category: | [[Category:Ophthalmology]] | ||
[[Category:Pediatrics]] | |||
Latest revision as of 09:32, 22 March 2026
Background
- Also known as preseptal cellulitis — infection anterior to the orbital septum
- Most often due to contiguous spread from sinusitis, skin infection, insect bite, or local trauma
- Most patients are <10 years old
- Rarely progresses to orbital cellulitis, but must be distinguished from it (see table below)
- Common organisms: S. aureus, S. pneumoniae, S. pyogenes, H. influenzae (in unvaccinated)
Periorbital vs Orbital Cellulitis
- Orbital cellulitis may mimic periorbital cellulitis early in its course
- Orbital cellulitis
- Ocular emergency
- Most often due to ethmoid sinusitis
- May also be due to orbital trauma, endophthalmitis, infection from teeth / middle ear
- Not caused by extension of periorbital cellulitis
- Periorbital cellulitis
- Usually benign
- Most often due to contiguous infection of soft tissues of face and eyelids
Clinical Features
.
- Eyelid swelling, erythema, tenderness, warmth
- +/- fever
- Key distinguishing features from orbital cellulitis (all ABSENT in preseptal):
- Proptosis
- Chemosis
- Globe displacement
- Limitation of extraocular movements
- Pain with eye movement
- Diplopia
- Vision loss
Differential Diagnosis
Periorbital swelling
Proptosis
- Normal IOP
- Orbital cellulitis
- Orbital pseudotumor
- Orbital tumor
- Increased IOP
- Retrobulbar abscess
- Retrobulbar emphysema
- Retrobulbar hemorrhage
- Ocular compartment syndrome
- Orbital tumor
No proptosis
- Periorbital cellulitis/erysipelas
- Dacryocystitis (lacrimal duct)
- Dacryocele/Dacryocystocele
- Dacryostenosis
- Dacryoadenitis (lacrimal gland)
- Allergic reaction
- Nephrotic Syndrome (pediatrics)
Lid Complications
- Blepharitis (crusts)
- Chalazion (meibomian gland)
- Stye (hordeolum) (eyelash folicle)
Other
- Subperiosteal abscess
- Orbital abscess
- Cavernous sinus thrombosis
- Conjunctivitis
- Contact dermatitis
- Herpes zoster
- Herpes simplex
- Sarcoidosis
- Granulomatosis with polyangiitis
Evaluation
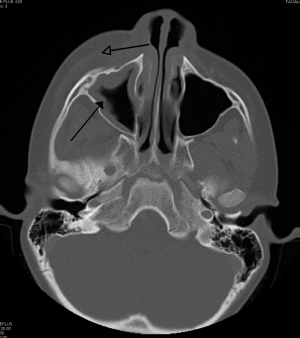
Periorbital cellulitis caused by a dental infection (also causing maxillary sinusitis).
- Visual acuity, pupil exam, extraocular movement assessment — essential to distinguish from orbital cellulitis
- CT orbit with IV contrast if:
- Equivocal exam (unable to fully assess proptosis, EOM, or pain with eye movement)
- Unable to accurately assess vision (e.g. age <1 year)
- Toxic-appearing or not improving on antibiotics
- Concern for orbital abscess (subperiosteal or orbital)
- Blood cultures if febrile or toxic-appearing
Management
Antibiotics
Outpatient
Treatment recommended for 5-7 days. If signs of cellulitis persist at the end of this period, treatment should be continued until the eyelid erythema and swelling have resolved or nearly resolved.
- TMP/SMX 1-2 double-strength tablets BID OR
- In children: TMP/SMX 8 to 12 mg/kg QD of the TMP component divided every 12 hours
- Clindamycin 300mg Q8H - In children: Clindamycin 30 to 40 mg/kg per day in three to four equally divided doses, maximum 1.8 grams per day
PLUS one of the following agents:
- Amoxicillin 875 mg BID OR
- In children: Amoxicillin 45-90 mg/kg per day divided every 12 hours
- Cefpodoxime 400mg BID OR
- In children: Cefpodoxime 10 mg/kg per day divided every 12 hours, max 200 mg
- Cefdinir 300 mg BID - In children: Cefdinir 14 mg/kg per day, divided every 12 hours, max daily 600 mg
Inpatient
- Vancomycin 15-20mg/kg IV BID + (one of the following)
- Ampicillin/Sulbactam 3 g IV q6hr OR
- Ticarcillin/Clavulanate 3.1 g IV q4h OR
- Piperacillin/Tazobactam 4.5 g IV q6h OR
- Ceftriaxone 2 g IV q12hr OR
- Cefotaxime 2 g IV q4h
Pediatric:
- Vancomycin 15mg/kg IV q6hrs + (one of the following)
- Ampicillin/Sulbactam 50mg/kg IV q6hrs (max 3g/dose) OR
- Piperacillin/Tazobactam 100mg/kg IV q8hrs (max 4.5g) OR
- Ceftriaxone 50mg/kg IV q12hrs (max 2g/dose) OR
- Cefotaxime 50mg/kg IV q6hrs (max 2g/dose)
Disposition
- Outpatient: Well-appearing, afebrile, mild disease, reliable follow-up in 24 hours
- Admit: Age <1 year, toxic-appearing, febrile, unable to tolerate PO, failed outpatient therapy, concern for orbital involvement
- Return precautions: Worsening swelling, fever, vision changes, pain with eye movement, inability to open eye




